Urticaria + Angioedema
This is a type 1 hypersensitivity reaction which gives a local release of histamine
– This increases the permeability of small capillaries and venules resulting in fluid shift to the extracellular space and pruritus, causing swelling of tissues.
Symptoms:
– Urticaria –> Swelling of the superficial dermis
– Presents as itchy red wheals which appear all over the body
– Angioedema –> deeper swelling of the dermis
– Presents as a swelling of tongue and lips
Management:
– Urticaria –> Antihistamines
– Angioedema –> Corticosteroids
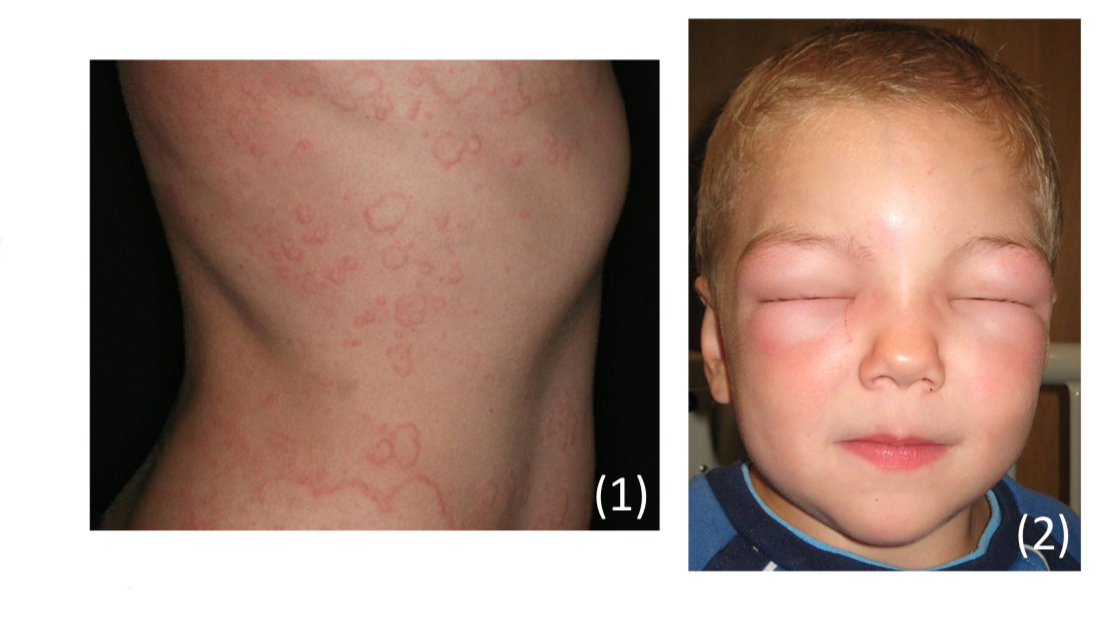
Hereditary angioedema
This is an autosomal dominant condition which occurs due to a deficiency in C1-INH (Complement 1 inhibitor)
– It also regulated the kallikrein system which involves clotting factors and precursors of bradykinin
– Deficiency leads to excessive release of bradykinin which is a vasodilator leading to oedema and inflammation
Symptoms
– Intermittent (1-2 week) spontaneous attacks which begin in childhood and worsen in adolescence
– Leads to angioedema which is worse for the first day then subsides, affecting limbs and abdomen.
– One third get a red rash (erythema marginatum) early before the attacks.
Diagnosis
– Low C4 with normal C1 and C3 –>If C4 is low, check C1-INH which will be low
Management
– If acute, give IV C1-inhibitor, kallikrein inhibitor or a BDKRRB2 antagonist
There are also group of 3 skin conditions which lie on a spectrum, rated by the degree of epidermal detachment:
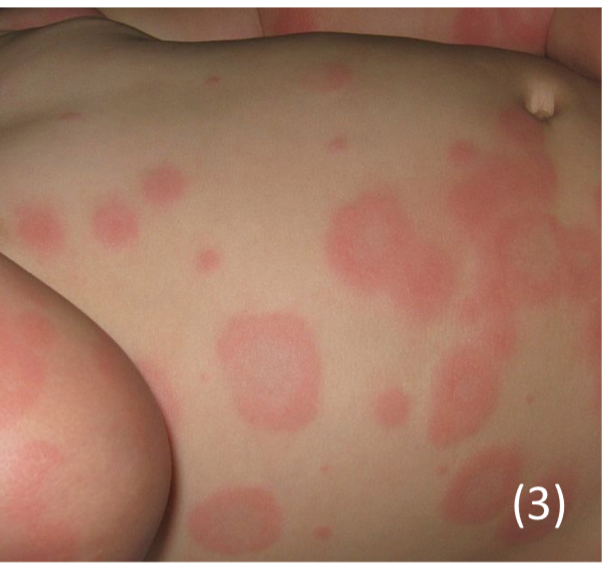
Erythema Multiforme
This is an acute inflammatory condition which results in target lesions (central necrosis surrounded by erythema) on hands, feet and the torso.
Two main types:
– Minor = Target lesions but no mucosal involvement
– Major = Target lesions with mucosal involvement, patients systemically unwell
Cause
– most common is Herpes Simplex virus
– Drugs –> Penicillin + NSAIDs + Sulphonamides + Anti-epileptics + Allopurinol
– Bacteria –> Mycoplasma (gives an atypical malaria with target lesions)
– Chronic inflammatory conditions –> Cancer, Sarcoidosis, SLE
Stevens Johnson Syndrome
This is a more severe form which is characterised by cutaneous necrosis with at least 2 mucosal sites involved
– It is a life threatening condition which causes necrosis and epidermal detachment.
– Due to a cytotoxic immune reaction causing keratinocyte apoptosis.
Symptoms
– Painful burning skin eruption, with loss of epidermis
– Patients get prodromal illness e.g. fever with URTI (upper resp tract infection) may precede rash
– Nikolsky sign positive – this is when slight rubbing of skin results in exfoliation of the epidermis
Toxic Epidermal Necrolysis
This is a life-threatening condition, which can be thought of as the most severe version of the previous conditions
– Usually it is called TEN when blisters cover >30% of the body
– The prognosis can be calculated using the SCORTEN scale
Symptoms
– Nikolsky sign positive
– Fever and tachycardia, but can lead to “skin failure,” with sepsis and hypovolaemic shock
Management
– Stop the cause and start IV antibiotics for sepsis
– IV immunoglobin or ciclosporin to stop the reaction, but steroids are usually avoided

